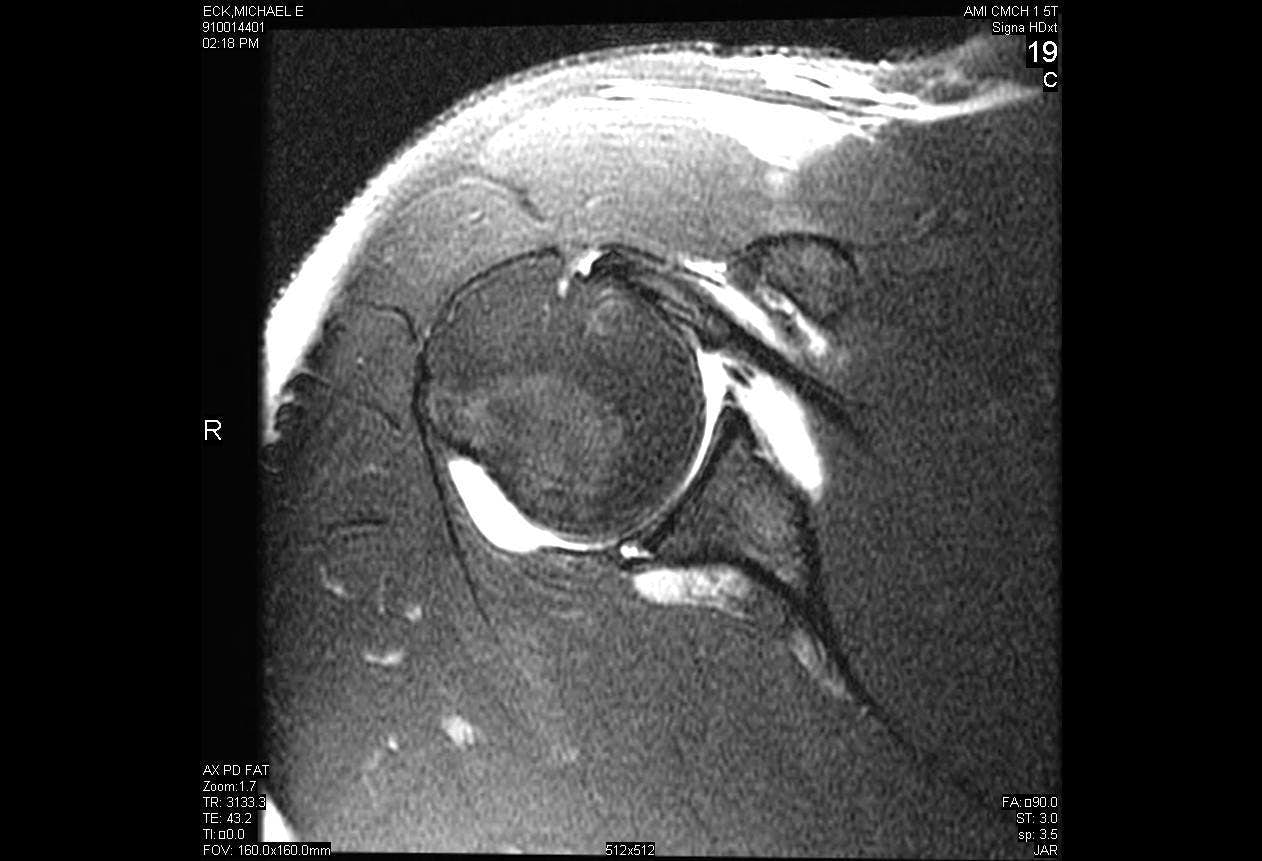
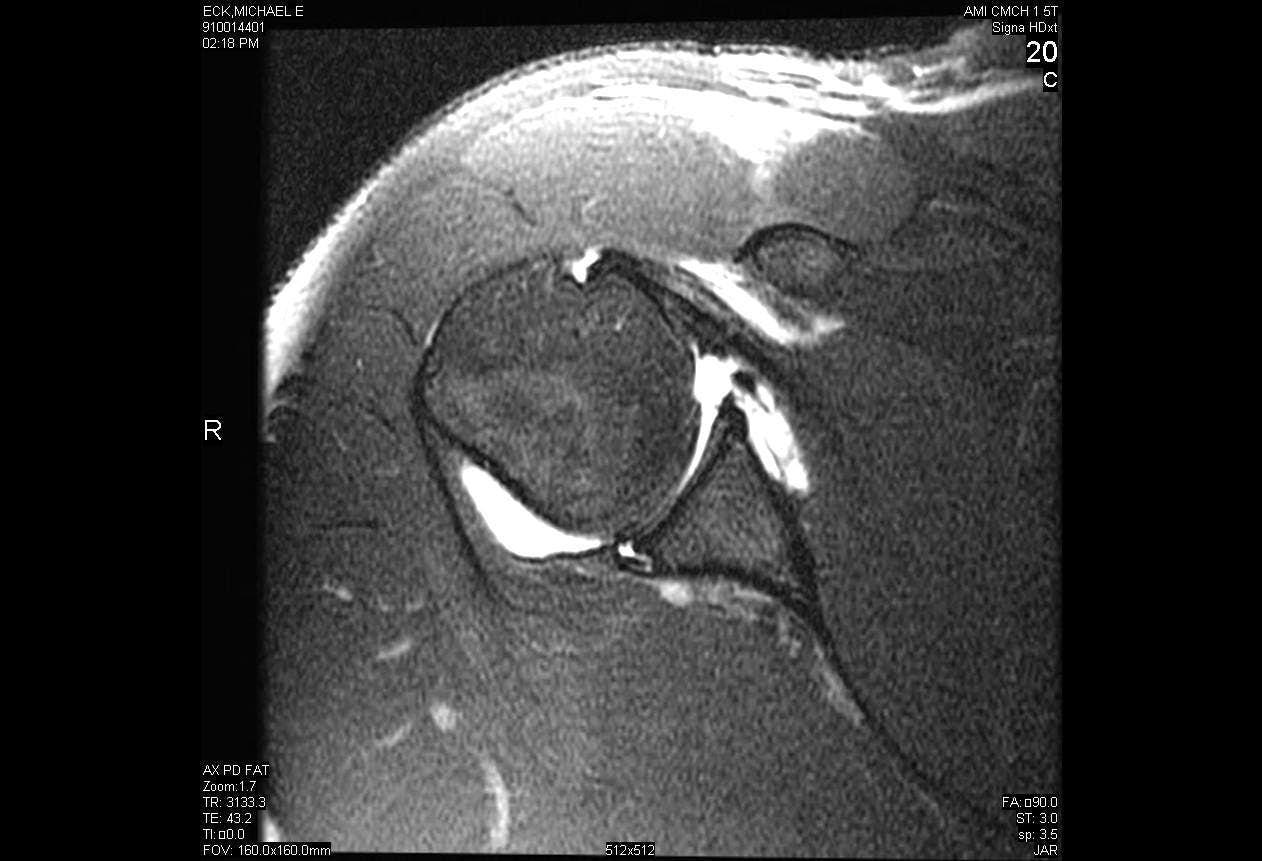
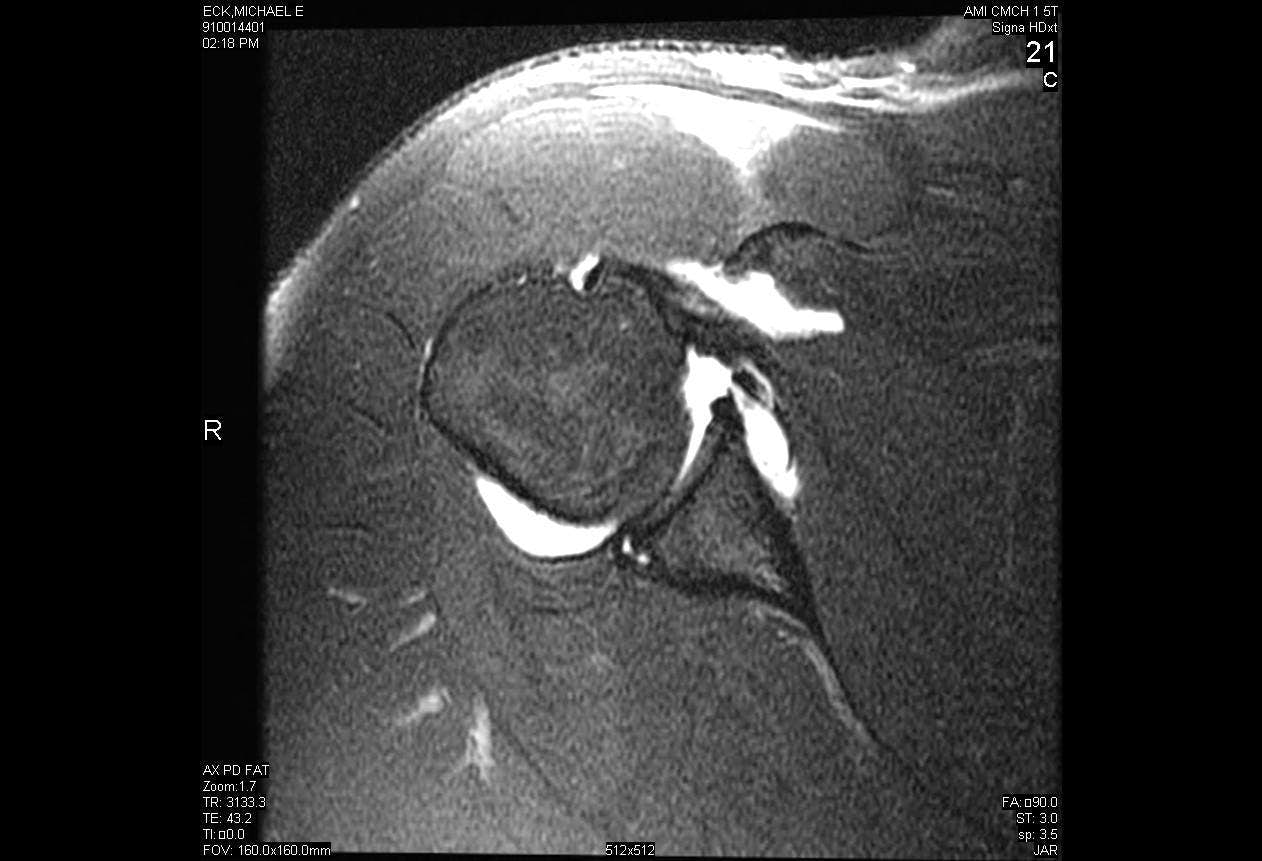
Arthroscopic Repair of Posterior Labral Tear with Paralabral Cyst Decompression
Main Text
Table of Contents
Posterior shoulder instability is a relatively rare phenomenon compared to anterior instability, comprising only 5-10% of all shoulder instability. Posterior instability most often occurs either as a result of high force direct trauma to the shoulder such as from a motor vehicle accident or indirect trauma such as from seizures or electrocution. Many cases of posterior shoulder instability are the result of micro-trauma that cause repetitive subluxation of the joint, ultimately compromising the shoulder in certain provocative positions. Surgical treatment of posterior instability is indicated only after an extended trial of rest and physical therapy has failed.
- What injury, trauma or repetitive shoulder motions have contributed to the current problem?
- Has the patient dislocated? If so, how many times and what was the mechanism?
- What maneuvers provoke pain? What is the patient’s reported pain severity on a scale of 1-10 for each of these maneuvers?
- What limitations in activity, if any, have occurred as a result of the instability?
- Is pain or instability present at rest? Does it interfere with sleep?
- Has the patient had conservative treatments including physical therapy, rest, anti-inflammatory medication, and if so, to what degree did these help?
- Palpate the shoulder for tenderness and document range of motion compared to the contralateral, normal extremity.
- Any restriction in motion should be compared to the contralateral shoulder.
- Differences between active and passive motion may indicate pain or capsular contracture.
- Impingement signs are tested to determine whether any associated rotator cuff tendinitis is present.
- If weakness is present during strength testing, it may be from deconditioning or from underlying rotator cuff or deltoid pathology.
- The degree of pathologic subluxation is assessed with a Load and Shift test, as well as any apprehension or pain experienced by the patient during provocative testing.
- Pathologic posterior subluxation is indicated by a positive Jerk Test
- A positive Kim test suggests a posteroinferior labral tear or subluxation.
- Circumduction test. A positive test result is highly suspicious of posterior subluxation or dislocation.
- Sulcus sign evaluation. A positive sulcus sign suggests multidirectional instability.
- The patient leaves the operating room in an abduction sling that can be removed for passive range-of-motion exercises at home.
- We allow 90 degrees of forward elevation and external rotation to 0 degrees by 4 weeks after surgery.
- The sling is discontinued 6 weeks after surgery and active assisted range-of-motion exercises and gentle passive range of motion exercises are progressed.
- Pain-free, gentle internal rotation exercises are instituted at 6 weeks.
- At 2 to 3 months after surgery, range of motion is progressed to achieve full passive and active range of motion.
- Stretching exercises can be instituted for any deficiency in motion at this point.
- After 4 months, the shoulder is often pain-free and eccentric rotator cuff strengthening is begun.
- At 5 months, isotonic and isokinetic exercises are advanced.
- At 6 months, throwing athletes undergo isokinetic strength testing. If 80% of the strength and endurance of the contralateral extremity is attained, a throwing program is begun.
- Full, competitive throwing is typically not attained until 12 months after surgery. Nonthrowing athletes are often released to a sport-specific program by 6 months, when 80% of their strength has returned.
- Recurrent instability
- Stiffness
- Infection
- Neurovascular injury
- Arthroscope, Stryker, Kalamazoo, MI
- 2.3mm Bio-Raptor Suture Anchors loaded with No. 2 Ultrabraid, Smith and Nephew, Andover, MA
- Spectrum Hook, Linvatec, Largo, FL
- 0 PDS Sutures, Ethicon, Somerville, NJ
References
- Blasier RB, Soslowsky LJ, Malicky DM, Palmer ML. Posterior glenohumeral subluxation: active and passive stabilization in a biomechanical model. J Bone Joint Surg Am. 1997;79(3):433-440. doi:10.2106/00004623-199703000-00018.
- Boyd HB, Sisk TD. Recurrent posterior dislocation of the shoulder. J Bone Joint Surg Am. 1972;54(4):779-786. doi:10.2106/00004623-197254040-00008.
- Bradley JP, Baker CL III, Kline AJ, Armfield DR, Chhabra A. Arthroscopic capsulolabral reconstruction for posterior instability of the shoulder: a prospective study of 100 shoulders. Am J Sports Med. 2006;34(7):1061-1071. doi:10.1177/0363546505285585.
- Gartsman GM, Hammerman SM. Superior labrum, anterior and posterior lesions: when and how to treat them. Clin Sports Med. 2000;19(1):115-124. doi:10.1016/S0278-5919(05)70299-4.
- Hawkins RJ, Koppert G, Johnston G. Recurrent posterior instability (subluxation) of the shoulder. J Bone Joint Surg Am. 1984;66(2):169-174. doi:10.2106/00004623-198466020-00002.
- Keppler P, Holz U, Thielemann FW, Meinig R. Locked posterior dislocation of the shoulder: treatment using rotational osteotomy of the humerus. J Orthop Trauma. 1994;8(4):286-292. doi:10.1097/00005131-199408000-00003.
- Kim SH, Ha KI, Park JH, et al. Arthroscopic posterior labral repair and capsular shift for traumatic unidirectional recurrent posterior subluxation of the shoulder. J Bone Joint Surg Am. 2003;85(8):1479-1487. doi:10.2106/00004623-200308000-00008.
- Kim SH, Park JS, Jeong WK, Shin SK. The Kim test: a novel test for posteroinferior labral lesion of the shoulder—a comparison to the jerk test. Am J Sports Med. 2005;33(8):1188-1192. doi:10.1177/0363546504272687.
- Kim SH, Park JC, Park JS, Oh I. Painful jerk test: a predictor of success in nonoperative treatment of posteroinferior instability of the shoulder. Am J Sports Med. 2004;32(8):1849-1855. doi:10.1177%2F0363546504265263.
- McLaughlin HL. Posterior dislocation of the shoulder. J Bone Joint Surg Am. 1952;34(3):584-590. doi:10.2106/00004623-195234030-00011.
- Pollock RG, Bigliani LU. Recurrent posterior shoulder instability: diagnosis and treatment. Clin Orthop Relat Res. 1993;291:85-96. https://journals.lww.com/clinorthop/Abstract/1993/06000/Recurrent_Posterior_Shoulder_Instability_.10.aspx.
- Silliman JF, Hawkins RJ. Classification and physical diagnosis of instability of the shoulder. Clin Orthop Relat Res. 1993;291:7-19. https://journals.lww.com/clinorthop/Abstract/1993/06000/Classification_and_Physical_Diagnosis_of.3.aspx.
- Tibone JE, Bradley JP. The treatment of posterior subluxation in athletes. Clin Orthop Relat Res. 1993;291:124-137. https://journals.lww.com/clinorthop/Abstract/1993/06000/The_Treatment_of_Posterior_Subluxation_in_Athletes.14.aspx.
- Walch G, Ascani C, Boulahia A, Nové-Josserand L, Edwards TB. Static posterior subluxation of the humeral head: an unrecognized entity responsible for glenohumeral osteoarthritis in the young adult. J Shoulder Elbow Surg. 2002;11(4):309-314. doi:10.1067/mse.2002.124547.
- Williams RJ III, Strickland S, Cohen M, Altchek DW, Warren RF. Arthroscopic repair for traumatic posterior shoulder instability. Am J Sports Med. 2003;31(2):203-209. doi:10.1177/03635465030310020801.
Cite this article
Tjoumakaris F. Arthroscopic repair of posterior labral tear with paralabral cyst decompression. J Med Insight. 2014;2014(3). doi:10.24296/jomi/3.