स्थानीय रूप से उन्नत रेक्टल कैंसर के लिए डायवर्टिंग लूप इलियोस्टोमी के साथ रोबोटिक लो एंटीरियर रिसेक्शन
Main Text
Table of Contents
यह वीडियो नियोएडजुवेंट फोल्फॉक्स-आधारित केमोरेडिएशन उपचार के बाद स्थानीय रूप से उन्नत मलाशय कैंसर के लिए एक रोबोट कम पूर्ववर्ती शोधन को दर्शाता है। रेक्टल ट्यूमर के लिए कम पूर्ववर्ती शोधन की सिफारिश की जाती है जिसमें स्फिंक्टर अतिक्रमण के बिना 1-सेमी डिस्टल मार्जिन प्राप्त किया जा सकता है। इस ऑपरेशन का एक प्रमुख घटक एक पूर्ण मेसोरेक्टल विच्छेदन है, जिसे रोबोटिक तकनीक के साथ हाइलाइट किया गया है। इस मामले में, हमारे रोगी के पास गुदा कगार से 6 सेमी ऊपर स्थित 2.6-सेमी ट्यूमर था, जिसका इलाज फोल्फॉक्स के आठ चक्रों के साथ किया गया था, जिसके बाद समेकित विकिरण चिकित्सा थी। एक रोबोट कम पूर्ववर्ती शोधन किया गया था, और अंतिम विकृति ने एक पूर्ण पैथोलॉजिकल प्रतिक्रिया का खुलासा किया।
कोलोरेक्टल कैंसर संयुक्त राज्य अमेरिका में कैंसर से संबंधित मौतों का तीसरा प्रमुख कारण है; हालांकि, फोल्फॉक्स-आधारित कुल नियोएडजुवेंट थेरेपी के अलावा मलाशय के कैंसर में बेहतर समग्र अस्तित्व का प्रदर्शन किया गया है। हालांकि कुछ रोगियों के पास चिकित्सा के बाद एक पूर्ण नैदानिक प्रतिक्रिया होगी, चल रही निगरानी की सिफारिश की जाती है। सर्जरी, जिसमें कम पूर्ववर्ती शोधन (एलएआर) या एब्डोमिनोपेरिनल रिसेक्शन (एपीआर) शामिल है, अवशिष्ट रोग या पुनरावृत्ति वाले सभी रोगियों के लिए अनुशंसित है। स्फिंक्टर कॉम्प्लेक्स के ऊपर निचले ट्यूमर के लिए एलएआर के लिए एक रोबोटिक दृष्टिकोण ऑन्कोलॉजिकल रिसेक्शन के दौरान मेसोरेक्टम का अद्वितीय विज़ुअलाइज़ेशन प्रदान करता है। इस वीडियो में, हम स्थानीय रूप से उन्नत रेक्टल कैंसर वाले रोगी के लिए एक रोबोट कम पूर्ववर्ती शोधन का प्रदर्शन करते हैं, जिसे नियोएडजुवेंट फोल्फॉक्स-आधारित केमोरेडिएशन के साथ इलाज किया गया था।
हमारी रोगी एक अन्यथा स्वस्थ 50 वर्षीय महिला है जिसे स्क्रीनिंग कोलोनोस्कोपी के लिए नवंबर 2020 की शुरुआत में प्रस्तुत किया गया था। गुदा कगार से लगभग 6-12 सेमी दूर बरकरार बेमेल मरम्मत जीन के साथ एक मामूली विभेदित रेक्टल एडेनोकार्सिनोमा की पहचान की गई और ल्यूमिनल परिधि के 30% पर कब्जा कर लिया गया। डिजिटल रेक्टल परीक्षा के दौरान गुदा कगार से द्रव्यमान लगभग 6-7 सेमी महसूस किया गया था। रोगी इस घाव से विशेष रूप से स्पर्शोन्मुख था।
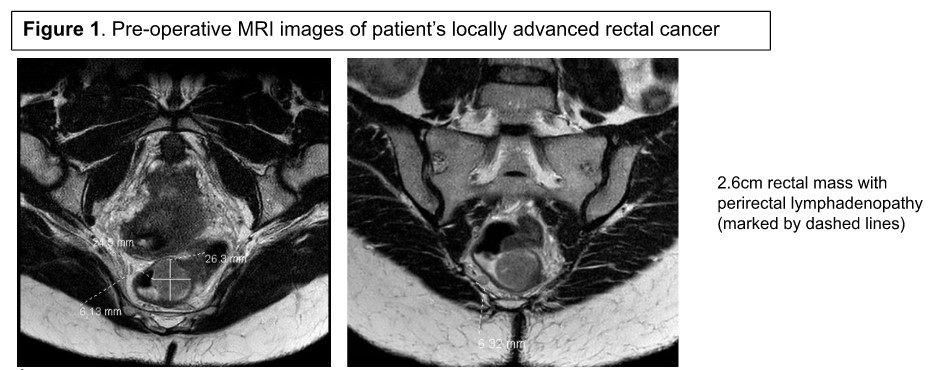
छाती, पेट और श्रोणि की अक्षीय इमेजिंग सहित स्टेजिंग वर्क-अप दूर या पेरिटोनियल मेटास्टेस के लिए नकारात्मक था। इसके अलावा, एक एमआरआई किया गया था, जिसने सीटी 3, सीएन 1, सीएम 0 (स्टेज IIIबी) रोग (चित्रा 1) के अनुरूप सीमावर्ती बढ़े हुए मेसोरेक्टल लिम्फ नोड्स के साथ एक अर्ध-परिधीय 2.6-सेमी रेक्टल द्रव्यमान दिखाया। उसका कार्सिनोएम्ब्रायोनिक एंटीजन (सीईए) स्तर 7.9 एनजी / एमएल था।
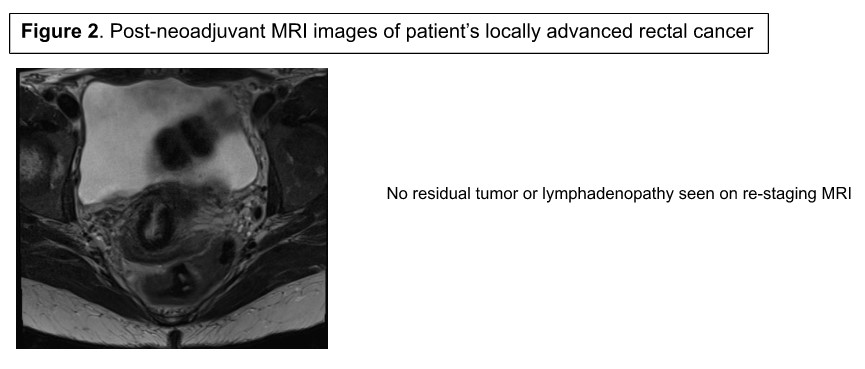
रोगी को नियोएडजुवेंट थेरेपी के लिए भेजा गया था, और जुलाई 2020 में फोल्फॉक्स-आधारित केमोरेडिएशन के आठ चक्र पूरे हुए थे। पुन: स्टेजिंग एमआरआई ने अवशिष्ट ट्यूमर या पेरिरेक्टल एडेनोपैथी का प्रदर्शन नहीं किया (चित्रा 2); हालांकि, एक लचीली सिग्मोइडोस्कोपी ने अवशिष्ट रोग के संकेत देने वाले ट्यूमर के स्तर पर एडेनोमेटस ऊतक दिखाया। अवलोकन बनाम सर्जरी के जोखिम और लाभों पर बहु-विषयक तरीके से चर्चा की गई थी, और रोगी रोबोटिक एलएआर के साथ आगे बढ़ने के लिए सहमत हुआ था। किसी भी एलएआर दृष्टिकोण के साथ, पर्याप्त शोधन के लिए कम से कम 12 लिम्फ नोड्स का 1-सेमी मार्जिन और पूर्ण मेसोरेक्टल एक्सिशन नमूना आवश्यक है।
रोगी को ऑपरेटिंग रूम में लाया गया और अपहरण किए गए हथियारों के साथ लापरवाह स्थिति में रखा गया। टेबल रिपोजिशनिंग के साथ शिफ्टिंग को रोकने के लिए बाहों और धड़ को बीन बैग और सुरक्षा पट्टियों के संयोजन के साथ सुरक्षित किया गया था। पोर्ट प्लेसमेंट की योजना तैयारी से पहले बनाई गई है और चित्रा 3 में विस्तृत है।
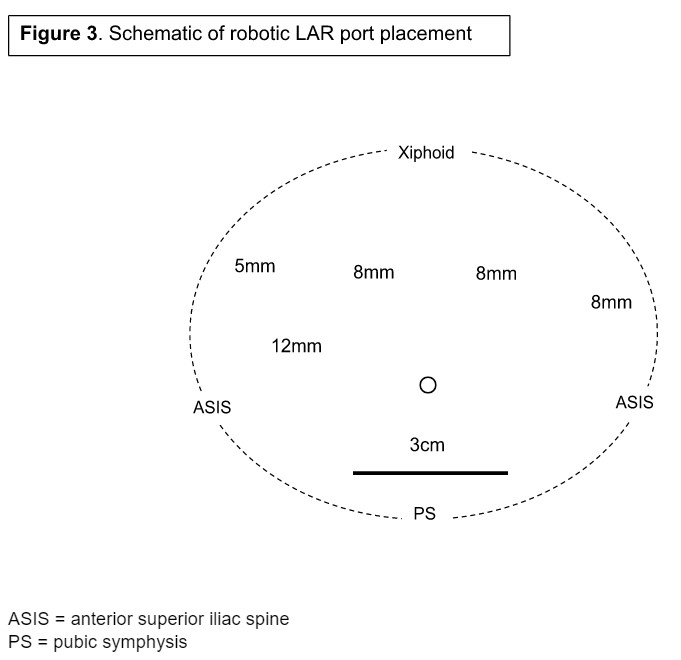
हमने जघन सिम्फिसिस के ऊपर लगभग 2 उंगली के चौड़ाई के साथ 3-सेमी फानेनस्टियल चीरा के साथ शुरुआत की। इस चीरा ने हमारे प्रारंभिक कैमरा पोर्ट और नमूना निष्कर्षण साइट दोनों के रूप में कार्य किया। एक एलेक्सिस घाव रक्षक डाला गया था, और बंदरगाह के माध्यम से एक 12 मिमी ट्रोकर रखा गया था। न्यूमोपेरिटोनियम की स्थापना की गई थी, और मनोगत मेटास्टैटिक बीमारी के लिए पेट का पता लगाया गया था। अतिरिक्त 8-मिमी बंदरगाहों को दाएं निचले क्वाड्रंट पोर्ट में प्रत्यक्ष विज़ुअलाइज़ेशन के तहत रखा गया था, एक हाथ की चौड़ाई पूर्ववर्ती इलियाक रीढ़ के साथ-साथ बाएं एपिगैस्ट्रिक क्षेत्र और बाएं ऊपरी चतुर्थांश में पेट के पार समान दूरी बिंदुओं पर। एक अंतिम 5-मिमी एयरसील वर्किंग पोर्ट को लंबर क्षेत्र में डाला गया था ताकि रिग्थ लोअर क्वाड्रंट और बाएं एपिगैस्ट्रिक पोर्ट के बीच त्रिकोणीय हो सके। ध्यान दें कि यदि डायवर्टिंग ओस्टोमी की योजना बनाई गई है, तो दाएं निचले क्वाड्रंट पोर्ट साइट का उपयोग अक्सर किया जाता है। डाविंची रोबोट को तब डॉक किया गया था, और काम करने वाले उपकरणों को ट्रोकार्स में डाला गया था। ध्यान दें कि दाईं निचली पोर्ट साइट को 12 मिमी तक बढ़ाया गया था और कैमरा पोर्ट के रूप में उपयोग किया गया था।
रोगी को अगली बार मामूली ट्रेंडेलेनबर्ग में दाईं ओर नीचे के साथ तैनात किया गया था ताकि इंट्राएब्डोमिनल सामग्री को जुटाने की सुविधा मिल सके। ओमेंटम को अनुप्रस्थ बृहदान्त्र में सेफलाड में बहा दिया गया था, और छोटे आंत्र को दाहिने ऊपरी चतुर्थांश में रखा गया था। हमारा विच्छेदन पार्श्व-से-औसत दर्जे के फैशन में सिग्मोइड बृहदान्त्र को पेल्विक ब्रिम और साइड वॉल से मुक्त करके शुरू हुआ। टोल्ट की सफेद रेखा को अवरोही बृहदान्त्र और इसके मेसेंटरी को समीपस्थ रूप से स्प्लेनिक फ्लेक्सर के स्तर तक बढ़ाने के लिए इंजेक्ट किया गया था।
एक बार जुटाने के बाद, हमने अगली बार हीन मेसेंटेरिक धमनी पेडिकल की पहचान की और पोत और रेट्रोपरिटोनियम के बीच एक विमान विकसित किया। इसे हमारे पूर्व पार्श्व-से-उपचारात्मक विच्छेदन तक विस्तारित किया गया था। अनजाने में चोट से बचने के लिए, विच्छेदन के इस हिस्से के दौरान मूत्रवाहिनी को स्पष्ट रूप से देखा गया था।
इसके बाद, हमने पहले पेरिटोनियम को ट्रेइट्ज़ के लिगामेंट के पार्श्व में जोड़कर मेडियल-टू-लेटरल विच्छेदन को पूरा करने के लिए सेफलाड को स्थानांतरित किया। अवर मेसेंटेरिक नस की पहचान की गई, घेर लिया गया, और एक ऊर्जा उपकरण के साथ लिया गया। औसत दर्जे के विच्छेदन के इस हिस्से को अनुप्रस्थ मेसोकोलन के नीचे और पार्श्व रूप से स्प्लेनिक फ्लेक्सर की ओर बढ़ाया गया था। स्प्लेनिक फ्लेक्सर को पूरी तरह से मुक्त करने और कोलोरेक्टल एनास्टोमोसिस के लिए पर्याप्त कोलोनिक लंबाई सुनिश्चित करने के लिए ओवरलाइंग ओमेंटल अटैचमेंट और गैस्ट्रोकोलिक लिगामेंट को इंजेक्ट किया गया था। फिर ध्यान औसत दर्जे के विच्छेदन पर लौट आया, जिसे आईएमए रूट की ओर पुच्छल रूप से बढ़ाया गया था।
विच्छेदन के समीपस्थ भाग के पूरा होने के साथ, हम हाइपोगैस्ट्रिक तंत्रिका जाल के सावधानीपूर्वक संरक्षण के साथ पैल्विक ब्रिम और साइडवॉल से समीपस्थ मलाशय को विच्छेदित करने के लिए आगे बढ़े। इसने रेट्रोपरिटोनियम से पूरे मेसोरेक्टम को ऊपर उठाने के लिए सही विमान में हमारे प्रवेश को सक्षम किया। हमने डगलस की थैली के चारों ओर पेरिटोनियल प्रतिबिंब को परिधीय रूप से जोड़कर और एक्स्ट्रापेरिटोनियल मलाशय को पुच्छल रूप से जुटाकर अपने विच्छेदन को पूरा किया। लचीला सिग्मोइडोस्कोपी यह सुनिश्चित करने के लिए किया गया था कि विच्छेदन अवशिष्ट ट्यूमर से नीचे था।
इसके बाद, ग्रीन लोड एंडो-जीआईए स्टेपलर की दो फायरिंग का उपयोग तब विच्छेदित डिस्टल मलाशय को सही करने के लिए किया गया था। कोलोनिक विच्छेदन को आईएमए को बाएं शूल टेक-ऑफ के ठीक बाहर जोड़कर पूरा किया गया था। आईसीजी एंजियोग्राफी में पर्याप्त छिड़काव की पुष्टि होने के बाद कोलोनिक मेसेंटरी को समीपस्थ ट्रांससेक्शन के स्तर तक विभाजित किया गया था। नमूने को तब फन्नेनस्टील चीरा के माध्यम से बाहरी बनाया गया था।
प्रस्तावित समीपस्थ ट्रांससेक्शन साइट को किसी भी पेरिकोलिक वसा से साफ कर दिया गया था और तेजी से विभाजित किया गया था। कोलोटॉमी के चारों ओर प्रोलीन सीवन को पिरोने के लिए एक स्वचालित पर्स स्ट्रिंग डिवाइस का उपयोग किया गया था। एक 28-फ्रेंच ईईए कोविडियन एनविल को लुमेन में डाला गया, प्रोलीन बांधा गया, और बृहदान्त्र पेरिटोनियल गुहा में लौट आया।
न्यूमोपेरिटोनियम को फिर से स्थापित किया गया था, और कोविडियन स्टेपलर को गुदा के माध्यम से डाला गया था। स्पाइक को रेक्टल स्टेपल लाइन के बीच में तैनात किया गया था, और स्पाइक के चारों ओर एक प्रोलीन पर्स स्ट्रिंग रखी गई थी। एनविल को स्टेपलर के अंत में जोड़ा गया और निकाल दिया गया। एनास्टोमोसिस को ओवरसेव करने के लिए एक पूर्ण मोटाई, चलने वाले वी-लॉक सीवन का उपयोग किया गया था। एनास्टोमोसिस की जांच करने और रिसाव परीक्षण करने के लिए लचीला सिग्मोइडोस्कोप डाला गया था।
क्योंकि ट्यूमर गुदा कगार के 7 सेमी के भीतर था और नियोएडजुवेंट थेरेपी के साथ इलाज किया गया था, एक अस्थायी डायवर्टिंग लूप इलियोस्टोमी तैयार किया गया था। इलियोकल वाल्व के लगभग 20 सेमी समीपस्थ इलियम के एक खंड की पहचान की गई और पकड़ लिया गया। दाहिने निचले चतुर्थांश बंदरगाह साइट के आसपास की त्वचा को उत्पादित किया गया था, और नरम ऊतकों को प्रावरणी में विच्छेदित किया गया था। प्रावरणी को क्रूसिएट फैशन में इंजेक्ट किया गया था, और मांसपेशी फाइबर विभाजित हो गए थे। इलियम के चयनित खंड को तब बिना किसी कठिनाई के एपर्चर के माध्यम से लाया गया था। स्टोमा टर्नबुल-ब्रुक फैशन में बाधित त्रिपक्षीय विक्रिल सीवन के साथ परिपक्व हो गया था।
रोगी ने प्रक्रिया को सहन किया और एक घटनारहित पोस्टऑपरेटिव रिकवरी हुई। उसे पोस्टऑपरेटिव दिन 3 पर घर से छुट्टी दे दी गई थी। अंतिम पैथोलॉजी ने बिना किसी अवशिष्ट ट्यूमर और 0/24 सकारात्मक लिम्फ नोड्स के साथ एक पूर्ण पैथोलॉजिकल प्रतिक्रिया का खुलासा किया। उन्हें फॉलो-अप में देखा गया और वह अच्छा प्रदर्शन कर रही हैं। सर्जरी के लगभग 12 सप्ताह बाद उसका ओस्टोमी उलट दिया जाएगा।
कई संभावित और पूर्वव्यापी समीक्षाओं ने कम पूर्ववर्ती शोधन में एनास्टोमोटिक रिसाव से जुड़े कारकों पर विचार किया है। कम रेक्टल ट्यूमर (गुदा कगार से <7 सेमी) और नियोएडजुवेंट केमोरेडिएशन के उदाहरणों में, एनास्टोमोटिक रिसाव दर अधिक होती है। 1, 2 इसलिए इन उदाहरणों में लूप इलियोस्टोमी के साथ अस्थायी डायवर्सन की सिफारिश की जाती है।
रोबोटिक दृष्टिकोण के लाभ के संदर्भ में, एक हालिया अध्ययन ने पूर्ण मेसोरेक्टल विच्छेदन की उच्च दर का प्रदर्शन किया, और लैप्रोस्कोपी की तुलना में कम लगभग पूर्ण या अपूर्ण विच्छेदन किया। हालांकि , यह याद रखना महत्वपूर्ण है कि विभिन्न दृष्टिकोणों में सर्जन अनुभव को कम पूर्ववर्ती शोधन दृष्टिकोण को निर्देशित करना चाहिए।
कोई विशेष उपकरण या प्रत्यारोपण नहीं।
खुलासा करने के लिए कुछ भी नहीं।
इस वीडियो लेख में संदर्भित रोगी ने फिल्माने के लिए अपनी सूचित सहमति दी है और वह जानता है कि जानकारी और छवियां ऑनलाइन प्रकाशित की जाएंगी।
कोई नहीं।
References
- स्किउटो ए, मेरोला जी, डी पाल्मा जीडी, सोडो एम, पिरोज़ी एफ, ब्राकेल यूएम, ब्राकेल यू। वर्ल्ड जे गैस्ट्रोएंटेरिओल। 2018;24(21):2247-60. दोई: 10.3748/ wjg.v24.i21.2247.
- पार्क जेएस, चोई जीएस, किम एसएच, एट अल। "लैप्रोस्कोपिक रेक्टल कैंसर एक्सिशन के बाद एनास्टोमोटिक रिसाव के लिए जोखिम कारकों का बहुआयामी विश्लेषण: कोरियाई लेप्रोस्कोपिक कोलोरेक्टल सर्जरी अध्ययन समूह"। एन सुर्ग। 2013;257(4):665-71. doi:10.1097/ SLA.0b013e31827b8ed9.
- बैक एसएच, क्वोन एचवाई, किम जेएस, हर एच, सोहन एसके, चो सीएच, किम एच रोबोटिक बनाम रेक्टल कैंसर के लैप्रोस्कोपिक लो एंटीरियर रिसेक्शन: एक संभावित तुलनात्मक अध्ययन का अल्पकालिक परिणाम। एन सुर्ग ओनकोल। 2009;16(6):1480-7. दोई: 10.1245/s10434-009-0435-3.
Cite this article
"स्थानीय रूप से उन्नत रेक्टल कैंसर के लिए लूप इलियोस्टोमी को डायवर्ट करने के साथ रोबोटिक लो एंटीरियर रिसेक्शन"। जे मेड इनसाइट। 2022;2022(343). दोई: 10.24296/


