Trigger Finger Release (Cadaver)
Main Text
Table of Contents
Stenosing flexor tenosynovitis of the digital flexor tendon sheath, also known as trigger finger, occurs when there is a size mismatch between the flexor tendon and the surrounding retinacular pulley system at the first annular (A1) pulley. The A1 pulley overlies the metacarpophalangeal (MCP) joint at the base of the finger. When the flexor tendon thickens or becomes inflamed, its ability to properly glide through the flexor tendon sheath becomes impaired. Thus, the tendon catches as the finger is flexed and extended. Trigger finger is a frequently encountered condition for most hand surgeons, and it often coexists with other disorders such as diabetes, rheumatoid arthritis, amyloidosis, and carpal tunnel syndrome.1–3 The cause is often idiopathic, though it has been speculated to result from overuse or repetitive movements of the finger.1,4 Conservative management includes activity modification, splinting, short-term nonsteroidal anti-inflammatory drugs (NSAIDs), corticosteroid injection, and other adjuvant therapies. This video demonstrates a surgical approach to the treatment of trigger finger via the open A1 pulley release procedure.
Patients often initially present with painless snapping, catching, or locking of the affected digit(s), followed by progression to painful episodes and spontaneous difficulty in digit extension. The pain is localized over the palmar aspect of the MCP joint and may radiate into the palm or distal finger. Patients may describe functional limitations in grasping objects and performing tasks requiring hand dexterity. Some patients awaken with the affected finger(s) locked in the flexed position, with gradual “unlocking” throughout the day.1 If severe, the finger may remain locked in position, requiring passive manipulation of the back into the relaxed state.
Physical exam reveals locking or clicking of the affected finger upon opening and closing the hand, though this may not occur consistently with every finger flexion. Thickening, swelling, or even a tender nodule is typically felt over the MCP joint.1,4 Patients complain of pain or tenderness around the MCP joint, often becoming reluctant to fully flex and extend the finger. This immobility may lead to a secondary contracture at the proximal interphalangeal (PIP) joint.1,5 As the palmar fascia overlying the tendon sheath gradually thickens, it can pull on the finger so that it remains in a flexed position. Additionally, it is not uncommon for multiple digits to be affected by trigger finger.6
If left untreated, patients with trigger finger will experience increasing pain and impaired finger mobility as the tendon becomes more thickened and inflamed. This developing disability may necessitate chronic use of painkillers in addition to appropriate accommodations and lifestyle adjustments.
Surgical treatment is reserved for patients who experience persistent pain and impairment, despite attempts at conservative therapy as well as at least one or two local corticosteroid injections. In these cases, surgical release of the A1 pulley can not only alleviate the patient’s pain, but also provide a long-term solution by reestablishing full range of motion in the affected digit(s).
During an open trigger finger release, the patient can be placed under local anesthesia alone, or with sedation or regional anesthesia. Local anesthesia is preferred as it allows the patient to participate with confirming release post-release.
This procedure is performed while the patient lies supine with his/her arm out to the side. The patient’s body and arm should be level. With the arm and hand relaxed, the volar aspect of the hand faces upward to allow the surgeon access to the necessary structures.
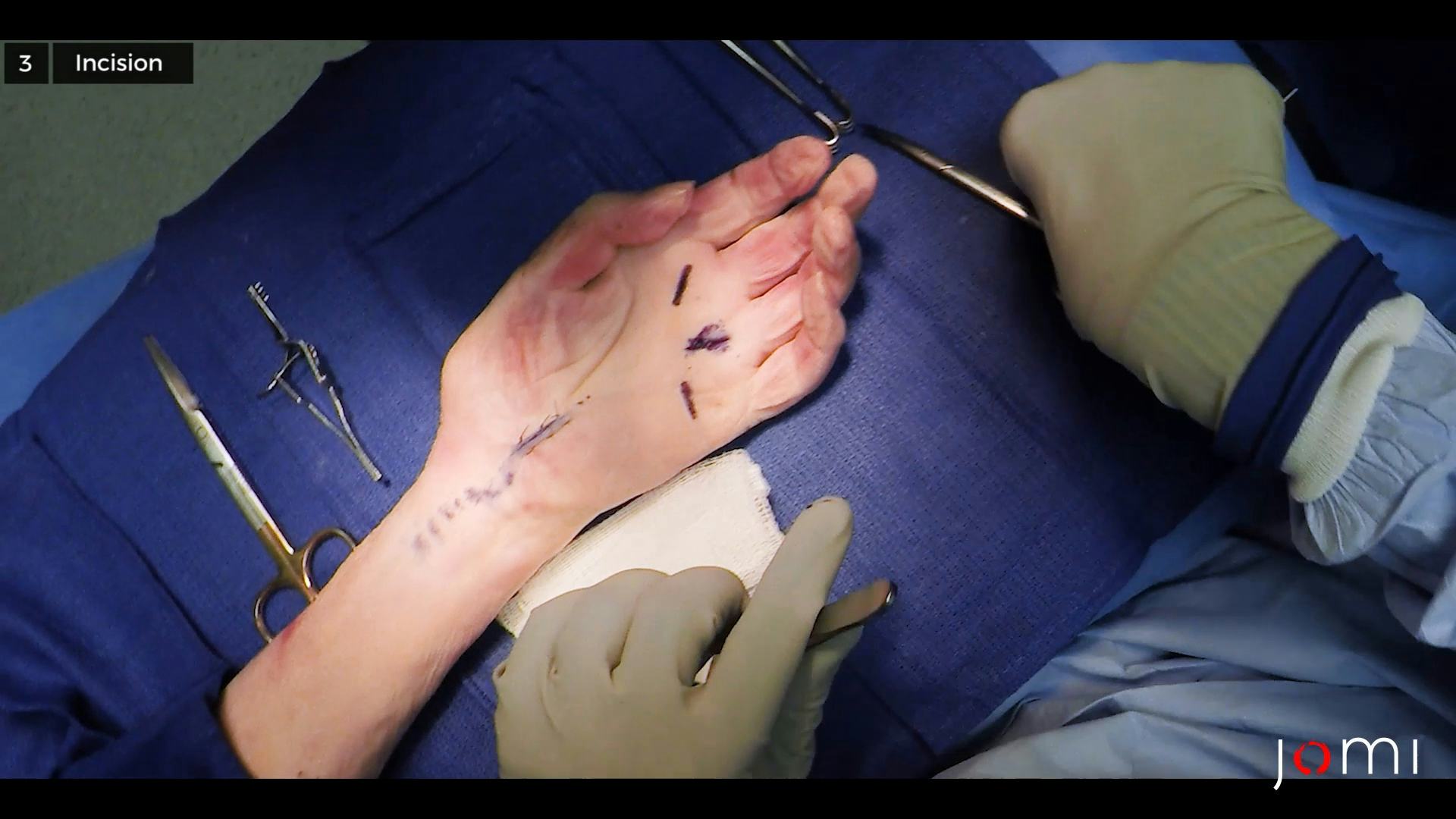
Trigger finger release may be performed openly or percutaneously. The open release of the A1 pulley, as shown here, represents the standard surgical approach for a trigger finger release. A pen is used to mark the incision site, which may be placed in various locations: (1) directly on top of the tendon, (2) obliquely in line with a palmar crease, or (3) proximally over the distal palmar crease. Though all of these locations may be effective in trigger finger release, a longitudinal incision directly over the tendon at the level of the MCP joint will provide the surgeon with maximal accessibility. The hand and arm are sterilized with antiseptic solution in order to decrease the risk of surgical site infection. A local anesthetic is injected.
A small incision (1.0-1.5 cm) is made on the volar aspect of the hand centered over the A1 pulley. The subcutaneous tissue is dissected to expose the underlying neurovascular structures. If the affected digit is the thumb, the radial digital nerve, which courses over the A1 pulley, should be identified and protected in order to prevent nerve injury. The A1 pulley is exposed and released longitudinally at least to the level of the A2 pulley. This is followed by subsequent decompression of the flexor tendon both proximally and distally. The release is confirmed by asking the patient to actively flex and extend the finger and no triggering should be confirmed visually by both the surgeon and patient. After confirming trigger finger release, the wound is irrigated and closed.
Postoperatively, any pain is preferably managed with non-opioids.7 Patients may resume normal daily activities immediately as tolerated, though they should avoid putting excess strain on the operated hand. Active range of motion exercises are encouraged. Once the wound is healed within one to two weeks, most patients can resume more vigorous activities, though some may need more time to recover. Sutures will be removed approximately two weeks postoperatively during the follow-up appointment.
Surgical complications are rare but include infection, flexor tendon bowstringing, tendon scarring, digital nerve injury, and continued triggering.1,6 Other adverse reactions may include dry mouth, nausea, vomiting, drowsiness, trouble urinating, itching, dizziness, sweating, coughing, and lethargy.7
Among the general population, the lifetime risk of developing trigger finger is 2.6%; however, this percentage rises to 10% in those with diabetes.8 It is most commonly seen in middle-aged women, particularly in the ring and/or middle fingers of the dominant hand.4,9 Trigger thumb occurs relatively frequently as well.8,10 The vast majority of cases are idiopathic, though trigger finger has been associated with carpal tunnel syndrome as well as endocrine and metabolic disorders.1–3,6
The majority of patients with trigger finger are initially treated with corticosteroid injections; however, the relapse rate for a single corticosteroid injection is approximately 29%.10 The successful treatment of trigger finger with these injections is highly variable, with reported rates ranging from 37% to 79.7%.2,9,11–14 The administration of multiple injections increases these percentages to above 90.2 Despite the aforementioned findings, corticosteroid injections are still recommended as the initial treatment for non-advanced trigger finger due to the conservative nature, simplicity, and low morbidity rates.
For patients with persistent trigger finger despite corticosteroid injections, standard treatment has been the open A1 pulley release described above.5 Often, the results of this surgery are excellent. With respect to success and recurrence rates, surgical intervention has been proven superior to corticosteroid injection.10 In one retrospective study, it was found that of a group of 59 patients who had undergone open release, 97% experienced complete resolution of triggering.2
Major complications after an open release are infrequent but include tendon bowstringing, nerve injury, ulnar deviation of the digits, and infection.2,15 In a group of 1598 patients undergoing open trigger finger release, less than 1% experienced persistent or recurrent triggering and none experienced nerve injury or serious infection.16 More commonly, patients experience minor complications such as decreased range of motion, scar tenderness, pain, and wound erythema.15 Those with diabetes are at greater risk of experiencing adverse events and often undergo a slower recovery than those without.16 Interestingly, male gender, sedation, and the use of general anesthesia during an open release may be associated with higher incidence of complications.17
Despite an increase in frequency of trigger finger release procedures, the best treatment remains unclear. Data suggest the failure and complication rates among patients undergoing either percutaneous release or open surgery are similar.5 The reported recurrence rate of trigger finger after surgical treatment (either open or percutaneous release) is around 3%.1,2,8 However, when compared to corticosteroid injections, percutaneous release resulted in fewer failures and higher patient satisfaction.5 The frequency of complications among these two groups was the same.5 In the case of trigger thumb, percutaneous release may be the less preferred surgical intervention due to the close proximity of the radial digital nerve.18
Ultimately, most recommend that corticosteroid injections should remain the first-line treatment for most cases of trigger finger; however, surgical treatment has been proven to be the “gold standard” of therapy if injections fail.2,19 Minor complications do occur relatively frequently, so patients should be fully informed of the potential outcomes. On the other hand, these surgical interventions rarely result in major complications and often provide definitive relief for those with persistent pain and functional impairment due to trigger finger.
Nothing to disclose.
Citations
- Blazar PE, Aggarwal R. Trigger finger (stenosing flexor tenosynovitis). UpToDate website. https://www.uptodate.com/contents/trigger-finger-stenosing-flexor-tenosynovitis. Accessed May 29, 2018.
- Turowski GA, Zdankiewicz PD, Thomson JG. The results of surgical treatment of trigger finger. J Hand Surg Am. 1997;22(1):145-149. doi:10.1016/S0363-5023(05)80195-9.
- Chammas M, Bousquet P, Renard E, Poirier JL, Jaffiol C, Allieu Y. Dupuytren's disease, carpal tunnel syndrome, trigger finger, and diabetes mellitus. J Hand Surg Am. 1995;20(1):109-114. doi:10.1016/S0363-5023(05)80068-1.
- Lunsford D, Valdes K, Hengy S. Conservative management of trigger finger: a systematic review. J Hand Ther. 2017. doi:10.1016/j.jht.2017.10.016.
- Wang J, Zhao JG, Liang CC. Percutaneous release, open surgery, or corticosteroid injection, which is the best treatment method for trigger digits? Clin Orthop Relat Res. 2013;471(6):1879-1886. doi:10.1007/s11999-012-2716-6.
- Ryzewicz M, Wolf JM. Trigger digits: principles, management, and complications. J Hand Surg Am. 2006;31(1):135-146. doi:10.1016/j.jhsa.2005.10.013.
- Ketonis C, Kim N, Liss F, et al. Wide awake trigger finger release surgery: prospective comparison of lidocaine, marcaine, and Exparel. Hand (N Y). 2016;11(2):177-183. doi:10.1177/1558944715627618.
- Lange-Rieß D, Schuh R, Hönle W, Schuh A. Long-term results of surgical release of trigger finger and trigger thumb in adults. Arch Orthop Trauma Surg. 2009;129(12):1617-1619. doi:10.1007/s00402-008-0802-8.
- Thorpe AP. Results of surgery for trigger finger. J Hand Surg Br. 1988;13(2):199-201. doi:10.1016%2F0266-7681_88_90138-6.
- Sato ES, Gomes dos Santos JB, Belloti JC, Albertoni WM, Faloppa F. Treatment of trigger finger: randomized clinical trial comparing the methods of corticosteroid injection, percutaneous release and open surgery. Rheumatology (Oxford). 2012;51(1):93-99. doi:10.1093/rheumatology/ker315.
- Schubert C, Hui-Chou HG, See AP, Deune EG. Corticosteroid injection therapy for trigger finger or thumb: a retrospective review of 577 digits. Hand (N Y). 2013;8(4):439-444. doi:10.1007/s11552-013-9541-6.
- Dala-Ali BM, Nakhdjevani A, Lloyd MA, Schreuder FB. The efficacy of steroid injection in the treatment of trigger finger. Clin Orthop Surg. 2012;4(4):263-268. doi:10.4055/cios.2012.4.4.263.
- Castellanos J, Muñoz-Mahamud E, Domínguez E, Del Amo P, Izquierdo O, Fillat P. Long-term effectiveness of corticosteroid injections for trigger finger and thumb. J Hand Surg Am. 2015;40(1):121-126. doi:10.1016/j.jhsa.2014.09.006.
- Wojahn RD, Foeger NC, Gelberman RH, Calfee RP. Long-term outcomes following a single corticosteroid injection for trigger finger. J Bone Joint Surg Am. 2014;96(22):1849-1854. doi:10.2106/JBJS.N.00004.
- Will R, Lubahn J. Complications of open trigger finger release. J Hand Surg Am. 2010;35(4):594-596. doi:10.1016/j.jhsa.2009.12.040.
- Bruijnzeel H, Neuhaus V, Fostvedt S, Jupiter JB, Mudgal CS, Ring DC. Adverse events of open A1 pulley release for idiopathic trigger finger. J Hand Surg Am. 2012;37(8):1650-1656. doi:10.1016/j.jhsa.2012.05.014.
- Everding NG, Bishop GB, Belyea CM, Soong MC. Risk factors for complications of open trigger finger release. Hand (N Y). 2015;10(2):297-300. doi:10.1007/s11552-014-9716-9.
- Uras I, Yavuz O. Percutaneous release of trigger thumb: do we really need steroid? Int Orthop. 2007;31(4):577. doi:10.1007/s00264-006-0288-3.
- Anderson B, Kaye S. Treatment of flexor tenosynovitis of the hand ('trigger finger') with corticosteroids: a prospective study of the response to local injection. Arch Intern Med. 1991;151(1):153-156. doi:10.1001/archinte.1991.00400010155024.
Cite this article
Xu V, Ilyas AM. Trigger finger release (cadaver). J Med Insight. 2021;2021(206.2). doi:10.24296/jomi/206.2.