Reconstruction of a Large Nasal Cutaneous Defect Using Nasolabial and Rhomboid Flaps
Main Text
Table of Contents
Resection of cutaneous malignancies may result in substantial skin defects. Often, skin grafting is a first-line option for reconstruction of such defects but may be limited by poor cosmetic outcomes and incomplete graft acceptance. Accordingly, skin flaps, tissue rearrangement techniques, and more complex procedures may be needed. This case report presents the successful use of a combination of nasolabial flap and rhomboid flap for reconstruction of a 3-cm × 2-cm left nasal sidewall and ala skin defect that remained following a basal cell cancer Mohs resection. The flaps were quickly and easily fashioned, did not require any special instruments, and resulted in a good cosmetic outcome. There were no wound complications and the flaps healed completely with excellent contour, texture, thickness, color match, and complete patient satisfaction. This case is an example of the technical aspects of successful planning, elevation, and inset of a nasolabial flap and rhomboid flap.
The origin of “reconstructive ladder” is believed to be in ancient Egyptian medical texts that were written between 2600 and 2200 BCE. The principle implies that the simplest effective technique should be considered first in reconstruction. The first description of the advancement flap was reported in Rome between 25 BCE and 50 CE.1
Rhomboid flap was first described by Alexander Alexandrovich Limberg in 1928. The traditional design consists of a parallelogram with 2 angles of 120° and 2 angles of 60°. This transpositional flap design consists of skin and subcutaneous tissue rotated around a pivot point into an adjacent defect.2, 3 This full-thickness cutaneous local flap typically relies on dermal-subdermal plexus blood supply.2, 4 The rhomboid flap is popular and can be used to reconstruct defects in most parts of the body. Over the years, several modifications have been reported.2, 5 Traditionally, rhomboid flaps have been safely used to reconstruct small- to moderately-sized skin defects.6, 7
This report presents a case where a large 3-cm × 2-cm left nasal defect was successfully reconstructed with a combined nasolabial flap and rhomboid flap.
An 82-year-old female presents with a several-month history of a nonhealing lesion of the left nasal ala. She had noted that the lesion was progressively getting larger, ulcerated, and more noticeable. She reported a past personal history for a basal cell skin cancer, but family history was negative for skin cancer. She noted moderate sun exposure and no sunblock use. Her past medical history was consistent with hypertension, kidney disease, and atrial fibrillation. She had undergone prior pacemaker placement. She was a nonsmoker and current medication included Rivaroxaban, Flecainide, and Diltiazem.
On physical examination, she was a Fitzpatrick class 2 skin type, elderly healthy woman with a height of 5 feet 3 inches, weight of 140 lbs, and body mass index of 24.8 kg/m3. The examination of the left nasal ala skin a 2-cm × 1.5-cm diameter, diffuse minimally-pigmented, scaly, suspicious lesion was noted. A punch biopsy was performed, and basal cell cancer was diagnosed. Given the size, location, and clinical findings, I referred the patient for Mohs extirpative excision. Following that procedure, she returned with negative margins, but with a large 3-cm × 2-cm defect of the nasal ala and left inferior nasal sidewall. Mucosa seemed largely intact, and the viability of the cartilage was unable to be assessed.
The plan was reconstruction with two local flaps: nasolabial flap from the superior portion of left nasal sidewall and rhomboid flap from the left medial cheek and nasolabial fold. The ear was also prepped for potential donor cartilage graft. The other potential treatment was full-thickness skin graft.
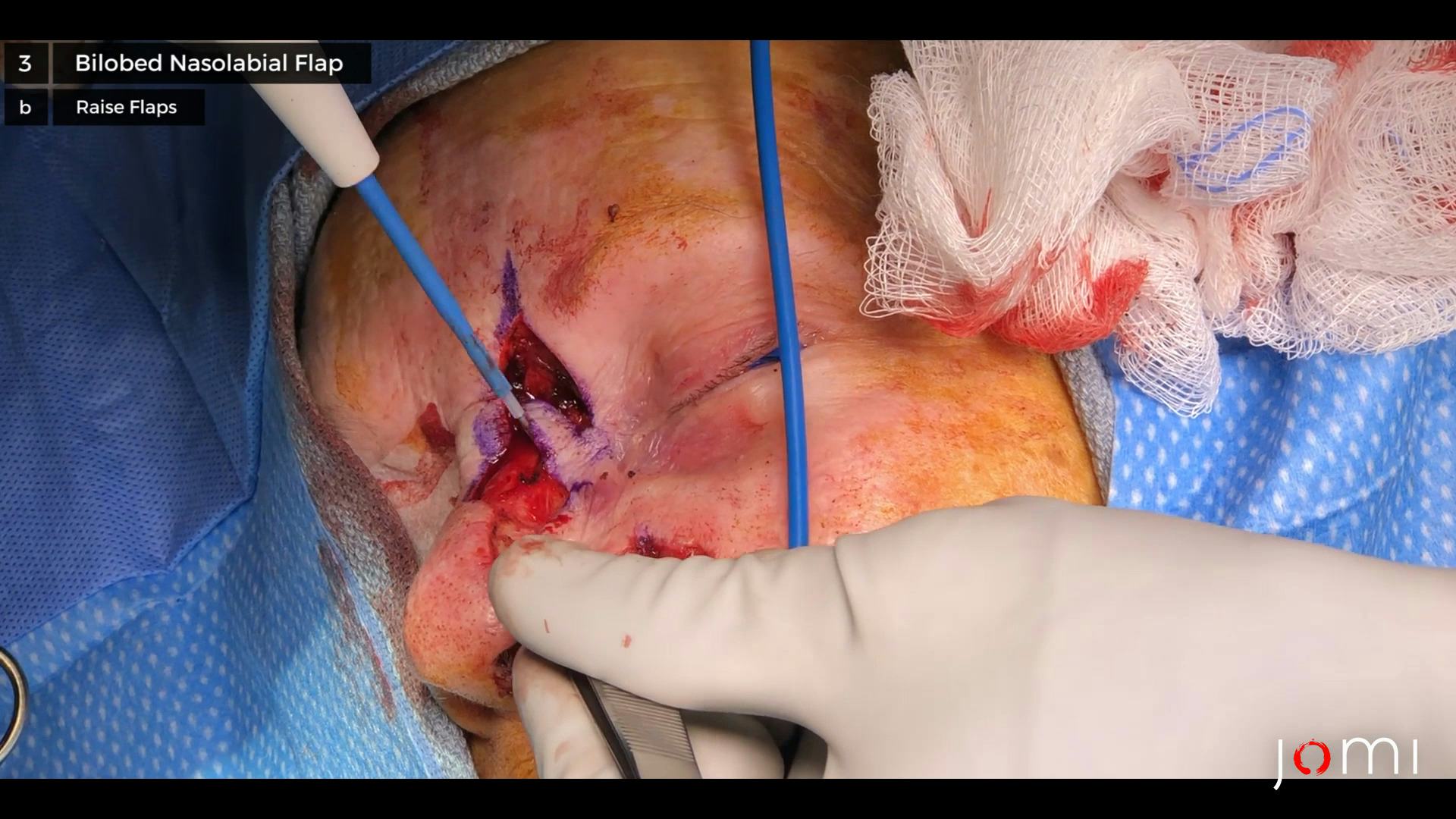
Under general anesthesia, a bilobed flap was marked adjacent to and superior to the left nasal sidewall defect. The mucosa defect was closed with two 5-0 chromic interrupted sutures. The left lower lateral cartilage was explored and was found to be intact. The nasolabial flap was raised at the level of the underlying cartilage and once mobilized was rotated inferiorly and medially to obliterate the anterior portion of the original defect. It was inset using 4-0 Biosyn interrupted sutures and 4-0 nylon interrupted sutures. At this point the anterior portion of the surgical defect was closed and reconstructed. However, the posterior portion was still open and needed a rhomboid flap. Accordingly, a rhomboid flap was marked along the inferior aspect of the defect. The incision was made, and the flap was raised at the level of the underlying fascia. The flap was rotated superiorly and medially to obliterate the defect. The flap was inset with 4-0 Biosyn interrupted sutures and 4-0 nylon interrupted sutures. At the conclusion of the procedure, both flaps were viable and the defect was obliterated. Antibiotic ointment and dry dressings were applied. The patient tolerated the procedure well and left the operating room in stable condition.
In the immediate postoperative period, the incisions were clean, dry, and intact. Both flaps remained viable. The healing was completely uneventful. Longterm follow-up also showed that the flaps healed completely without problems or limitations.
Plastic surgery is a unique specialty where numerous acceptable options may exist for the reconstruction of a single defect.6 Each reconstruction should be tailored to the unique characteristics of the defect, patient expectations, and surgeon's experience.8 The reconstructive ladder framework suggests using first the simplest technique that proves effective.1, 8 At times, primary closure and skin grafts may lead to distortion, contour deformity, or unacceptable scarring. Such instances, even for small lesions, are more suitable for skin flaps.6, 9
An elliptical excision with primary closure may leave a central depression, flat contour, and “dog ear” peaks on both corners.5, 10 To avoid this deformity, an incision length-to-width ratio of 3:1 is required, creating a longer linear scar.10, 11 Unfortunately, larger portions of healthy skin around the defect are sacrificed, and aesthetic outcomes may be compromised.10, 11 Well-designed local flaps avoid these limitations.6
Nasolabial and Rhomboid flap designs are chosen such that the line of donor closure is placed along the line of maximal extensibility closure resulting in better distribution of tension. The participation of surrounding skin also reduces tension.5, 6 Less tension means improved chances of healing and less risk of distortion of adjacent anatomic architecture.6 The “broken” geometric final scar appearance also makes it less noticeable.6, 12 A recent meta-analysis comparison with primary closure, for sacrococcygeal pilonidal surgeries, showed rhomboid flaps resulted in a lower relative risk of dehiscence and wound infection.13
The presented case further highlights a successful reconstruction of a large 3-cm × 2-cm cutaneous left nasal sidewall and ala defect. Primary closure was simply not an option given the local size of the defect and the potential distortion of key structures. A skin graft would have left a permanent, prominent, hypopigmented, depressed area at the recipient site.
Our results are consistent with other reports in the literature that note the successful applicability of nasolabial and rhomboid flaps in almost all parts of the body. We believe for high safety, high patient satisfaction, and best cosmetic outcomes, rhomboid and other local flaps should be considered as a first-line reconstructive strategy for covering defects of various sizes and locations.
The nasolabial and rhomboid flap design is simple, flap elevation is quick, and no special instrumentation is required, making these techniques suitable even in a resource-limited environment.
This case details the operative technical aspects of evaluation of defect, flap design, flap markings, flap elevation, flap rotation, flap inset, and postoperative management to aid readers in utilizing this technique. The final flap healed with excellent contour, texture, thickness, and color match.
No special instrumentation needed.
Nothing to disclose.
The patient referred to in this video article has given their informed consent to be filmed and is aware that information and images will be published online.
Citations
- Kang AS, Kang KS. Expanding the scope of rhomboid flap: large cutaneous defect reconstruction. Case report. Ann Med Surg (Lond). 2021 Jan 26;62:369-372. doi:10.1016/j.amsu.2021.01.082.
- Aydin O.E., Tan O., Algan S., Kuduban S.D., Cinal H., Barin E.Z. Versatile use of rhomboid flaps for closure of skin defects. Eurasian J Med. 2011;43(1):1-8. doi:10.5152/eajm.2011.01.
- Chasmar LR. The versatile rhomboid (Limberg) flap. Can J Plast Surg. 2007;15(2):67-71. doi:10.1177/229255030701500207.
- Alvarez GS, Laitano FF, Siqueira EJ, Oliveira MP, Martins PDE. Use of the rhomboid flap for the repair of cutaneous defects. Rev Bras Cir Plást. 2012;27(1):102-107.
- Quaba AA, Sommerlad BC. "A square peg into a round hole": a modified rhomboid flap and its clinical application. Br J Plast Surg. 1987 Mar;40(2):163-70. doi:10.1016/0007-1226(87)90189-5.
- Kang AS, Kang KS. Rhomboid flap for large cutaneous trunk defect. Plast Reconstr Surg Glob Open. 2020 Jun 18;8(6):e2932. doi:10.1097/GOX.0000000000002932.
- Kang AS, Kang KS. Rhomboid flap: indications, applications, techniques and results. A comprehensive review. Ann Med Surg (Lond). 2021 Jul 7;68:102544. doi:10.1016/j.amsu.2021.102544.
- Janis JE, Kwon RK, Attinger CE. The new reconstructive ladder: modifications to the traditional model. Plast Reconstr Surg. 2011 Jan;127 Suppl 1:205S-212S. doi:10.1097/PRS.0b013e318201271c.
- Borges AF. The rhombic flap. Plast Reconstr Surg. 1981 Apr;67(4):458-66. doi:10.1097/00006534-198104000-00007.
- Kang AS, Kang KS. A systematic review of cutaneous dog ear deformity: a management algorithm. Plast Reconstr Surg Glob Open. 2020 Sep 23;8(9):e3102. doi:10.1097/GOX.0000000000003102.
- Tilleman TR, Neumann MH, Smeets NW, Tilleman MM. Waste of skin in elliptical excision biopsy of non-melanomatous skin cancer. Scand J Plast Reconstr Surg Hand Surg. 2006; 40:352-356. doi:10.1080/02844310601011934.
- Kang AS, Kang KS. Rhomboid flap: indications, applications, techniques and results. A comprehensive review. Ann Med Surg (Lond). 2021 Jul 7;68:102544. doi:10.1016/j.amsu.2021.102544.
- Horwood J, Hanratty D, Chandran P, Billings P. Primary closure or rhomboid excision and Limberg flap for the management of primary sacrococcygeal pilonidal disease? A meta-analysis of randomized controlled trials. Colorectal Dis. 2012 Feb;14(2):143-51. doi:10.1111/j.1463-1318.2010.02473.x.
Cite this article
Kang AS. Reconstruction of a large nasal cutaneous defect using nasolabial and rhomboid flaps. J Med Insight. 2023;2023(323). doi:10.24296/jomi/323.